Sinus infections, medically known as sinusitis, are common respiratory disorders that can cause a variety of symptoms. Aside from the usual congestion and discomfort, sinusitis can also lead to ear pain, which may result in a pressure imbalance and potential hearing loss.
What is Sinusitis?
Sinusitis is an inflammation of the sinus passages caused by viruses, bacteria, or fungi. These infections can cause sinus lining edema, resulting in symptoms such as nasal congestion, face discomfort, sinus headaches, and a sore throat. Symptoms of sinusitis also include sinus congestion, which can lead to sinus pressure and pain.
When sinusitis is acute, it is often referred to as acute sinusitis and can cause significant discomfort. The sinus inflammation associated with this condition can block the normal drainage of the sinuses, leading to increased pressure within the air-filled cavities of the sinus passages.
Sinusitis Symptoms and Nasal Congestion
- Facial pain and pressure, especially around the nose, eyes, and forehead
- Nasal congestion and discharge
- Runny or stuffy nose
- Fever
- Fatigue
- Loss of smell or taste
- Bad breath
- Ear pressure
Causes of Sinusitis
- Viral or bacterial infections (common cold)
- Allergies
- Deviated septum
- Polyps in the nasal passages
- Certain medications
- Environmental irritants like smoke or dust
Can Sinus Infections Lead to Hearing Loss?
The answer is yes, but not directly. Sinusitis does not usually permanently harm the delicate components of the inner ear that are crucial for hearing. It can, however, cause temporary hearing loss in a few ways:
Fluid buildup: When the sinuses become inflamed, they create extra mucus, which can clog the Eustachian tube, a tiny conduit that connects the middle ear to the back of the throat. This trapped fluid interferes with sound wave transmission, resulting in muted hearing, ear fullness, and difficulties comprehending speech. This congestion and discomfort can significantly affect the affected ear.
Inflammation and swelling: In extreme cases, inflammation can migrate to the middle ear, damaging the eardrum and ossicles (tiny bones that transmit sound). This can exacerbate hearing loss and cause ear pain due to the blockage of the Eustachian tube.
Ear canal blockage: The inflammation can also lead to fluid buildup and blockage in the ear canal, further contributing to hearing issues and discomfort.
Ear infections: Untreated chronic sinusitis increases the risk of secondary ear infections (otitis media), which can potentially cause temporary hearing loss.
Middle ear infection: Sinusitis can lead to middle ear infections, causing symptoms such as ear congestion, dizziness, pain, and fluid drainage.
Sinus and ear infections: There is a significant relationship between sinus and ear infections, as both conditions can exacerbate each other and lead to more severe symptoms. Seeking treatment is crucial to prevent and manage these interconnected issues.
Is Sinusitis-Related Middle Ear Hearing Loss Permanent?
Fortunately, sinus-induced hearing loss is usually temporary. Hearing usually returns to normal within a few days or weeks after the infection clears and the Eustachian tube opens. However, if the illness is severe or ignored, it might result in problems such as:
- Chronic middle ear infections resulting in permanent hearing loss
- Otitis media with effusion (fluid accumulation in the middle ear) is a kind of otitis media.
- Scarring in the middle ear, resulting in irreversible hearing loss
Types of Hearing Loss
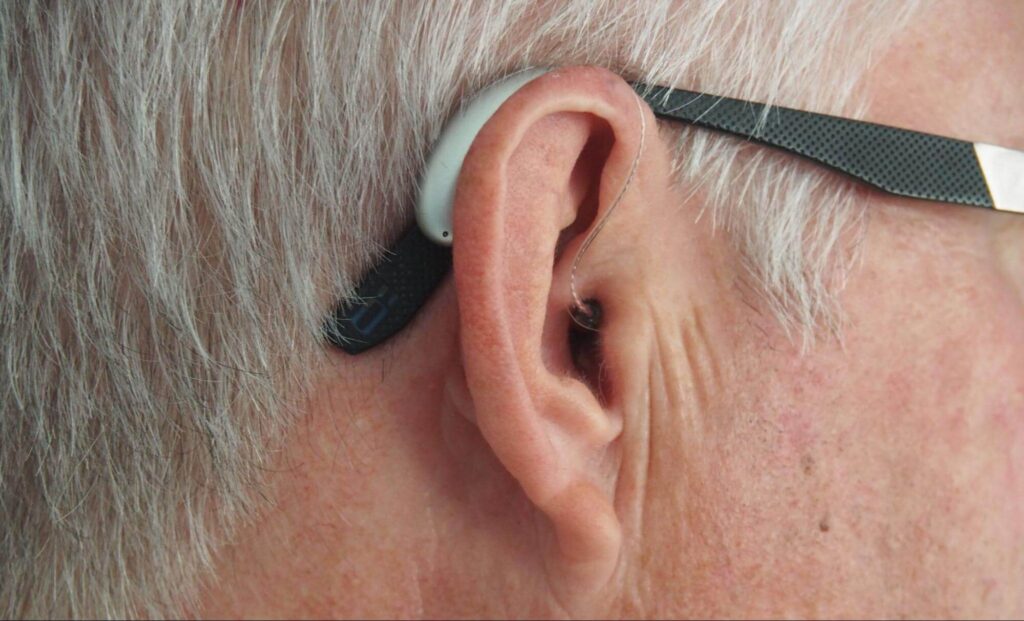
Two main types of hearing loss can occur from sinus infections:
Conductive Hearing Loss
When sound is not correctly carried via the outer ear, tympanic membrane (eardrum), or middle ear (ossicles), it results in conductive hearing loss. This form of hearing loss is usually transient and is caused by fluid accumulation in the middle ear as a result of a sinus infection.
The fluid inhibits the ossicles from vibrating properly, resulting in hearing loss. Sinusitis-related conductive hearing loss is often mild to moderate in severity. Once the sinus infection has cleared, it may vary and improve.
Sensorineural Hearing Loss
Damage to the inner ear (cochlea) or auditory nerves causes sensorineural hearing loss. This form of hearing loss is usually permanent. Although sensorineural hearing loss caused by a sinus infection is uncommon, it can occur if the infection progresses beyond the sinus cavities to the inner ear or auditory nerve.
Inflammation caused by the infection destroys the delicate tissues involved in hearing. Sinusitis-related sensorineural hearing loss causes more substantial, permanent hearing impairment.
Treating Sinusitis to Alleviate Hearing Loss
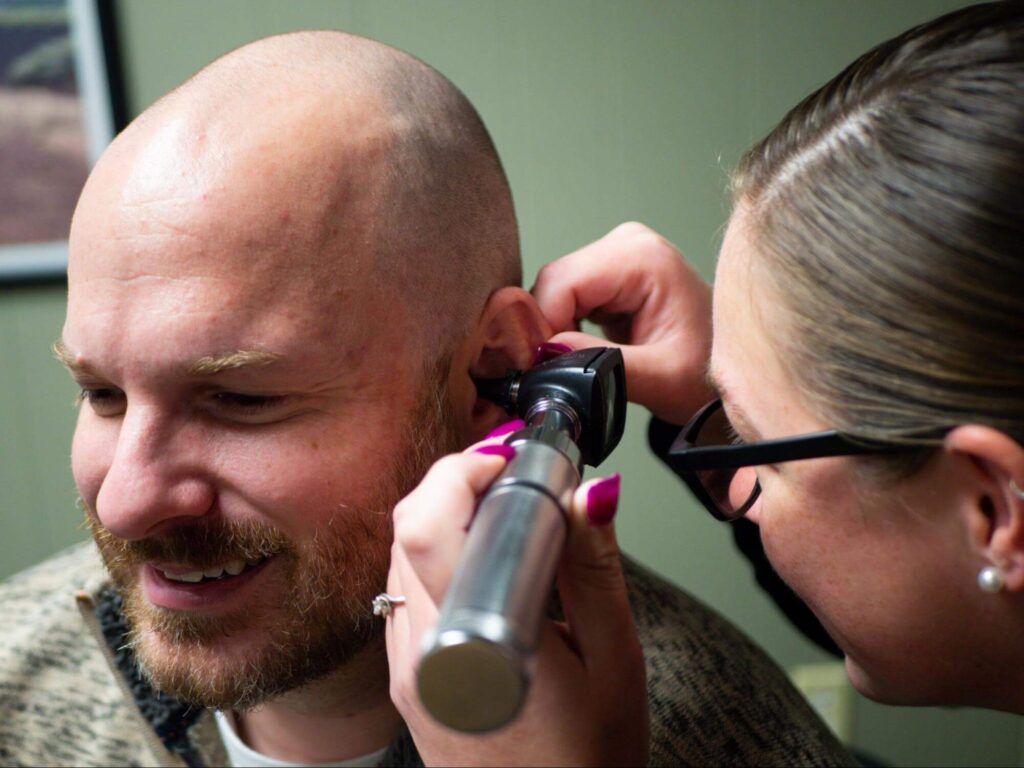
There are several sinusitis treatment methods available, some of which may help to reduce related hearing loss. Treating sinusitis also helps ear pain caused by the infection.
Medications
Bacterial sinus infections are frequently treated with antibiotics. These are intended to clean out infection and decrease inflammation in the sinuses, perhaps relieving pressure on the Eustachian tubes and middle ear.
Decongestants can also be used to relieve congestion and unblock closed passageways. Corticosteroid nasal sprays work to reduce swelling and mucus production.
OTC pain medicines such as acetaminophen and ibuprofen can also help control the discomfort and suffering caused by the sinus infection. It is critical to take drugs exactly as directed to properly treat sinusitis.
Surgery
If drugs do not relieve a persistent or severe sinus infection, surgery may be indicated. Endoscopic sinus surgery is the most frequent method, and it includes an ear, nose, and throat expert utilizing tiny telescopes and devices to clear up clogged sinus airways.
This increases nasal drainage and ventilation while also eliminating diseased tissues. Sinus surgery is often performed as an outpatient treatment with a brief recovery period. The underlying cause of recurrent sinusitis can be effectively treated with surgery.
Other Treatments
- Nasal sprays: Steroid nasal sprays can help to decrease inflammation and edema in the nasal passages and sinuses.
- Warm compresses: Applying warm compresses to your face might help reduce discomfort and facilitate drainage.
- Humidifiers: Adding moisture to the air can help release mucus and make sinus clearing easier.
- Elevation: Sleeping with your head slightly raised can help keep nasal discharge out of your middle ear.
Preventing Sinusitis-Related Hearing Loss

Here are some tips to help you avoid sinus infections and reduce your chance of hearing loss:
- Hand washing should be done regularly.
- Avoid irritants such as secondhand smoke.
- Keep hydrated.
- To keep your nasal passages wet, use a saline nasal spray.
- Effectively manage allergies and chronic diseases.
- Exercise regularly to strengthen your immune system
- Use a humidifier if the air in your home is dry. While sleeping, use a cool mist humidifier in your bedroom to provide moisture to the air.
- Obtain immunizations. To avoid respiratory infections, keep up to date on vaccinations such as the flu shot and pneumonia vaccine.
- Consult an ENT if you have frequent or severe sinus infections to ensure that you are appropriately diagnosed and treated.
To manage sinus related issues, a healthcare professional can provide a proper diagnosis to determine whether the cause is a viral or bacterial infection. If it is bacterial, antibiotics may be prescribed. Treatment often aims to relieve sinus pressure and reduce inflammation. This can include the use of decongestants, nasal sprays, and sometimes ear drops to alleviate associated ear discomfort. Managing these symptoms effectively can prevent further complications and promote better overall health.
If your hearing loss persists or worsens, see a doctor right away since timely treatment can avoid consequences.



